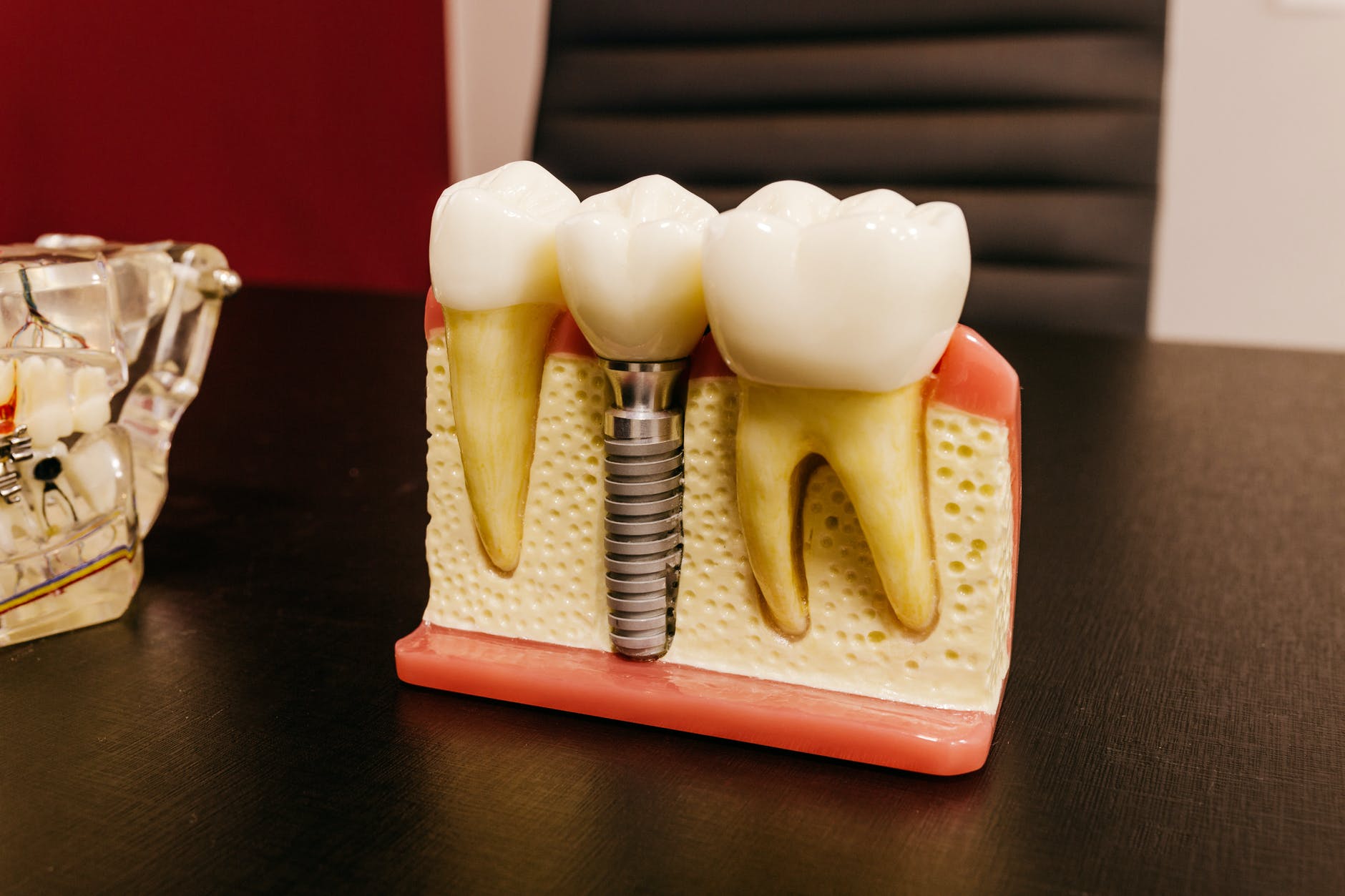
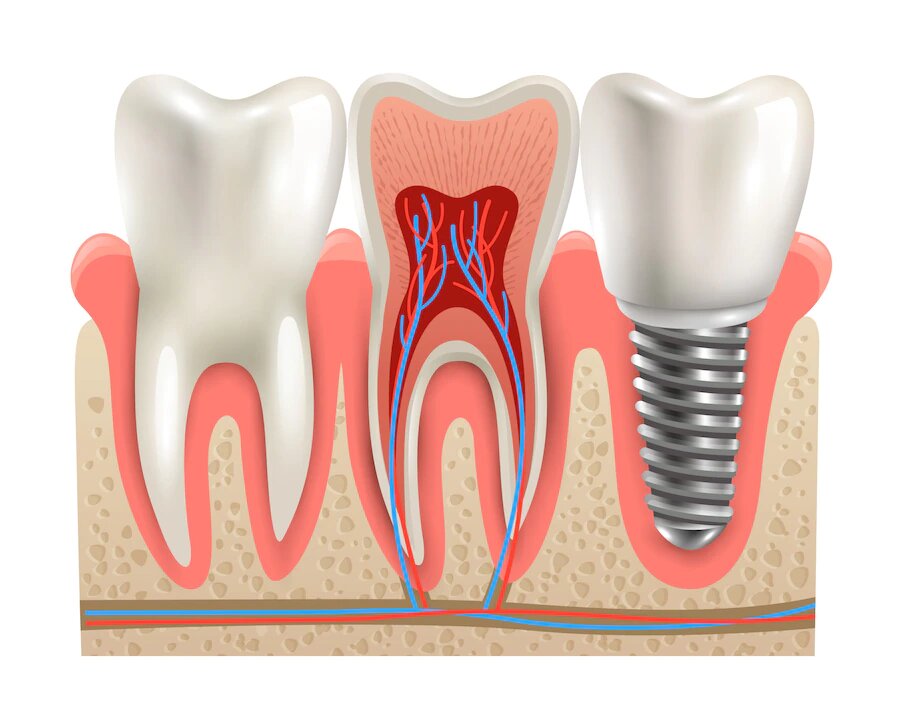
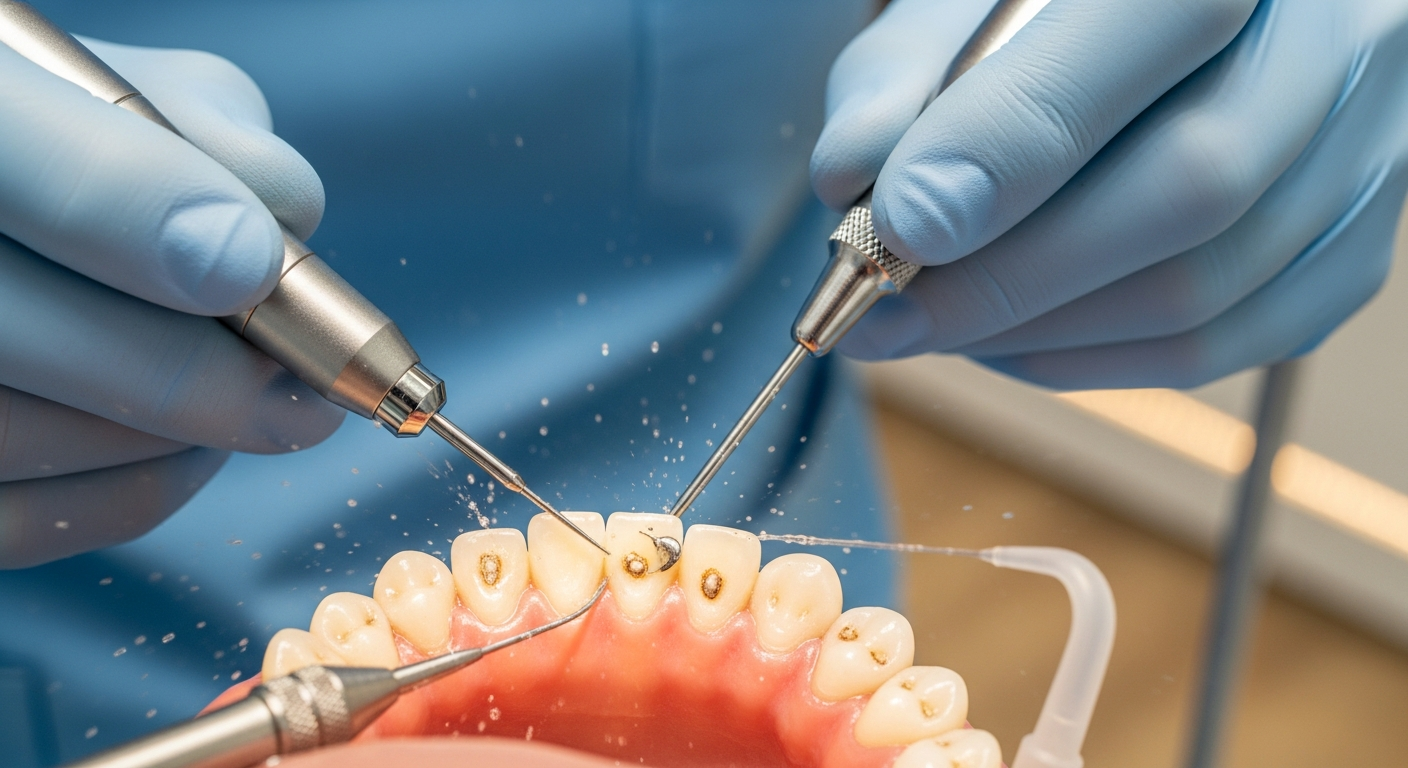
How Dentists Treat Gingivitis?

Dentists treat gingivitis primarily through professional cleaning and scaling to remove plaque and tartar. If caught early, gingivitis is fully reversible. Untreated, it progresses to periodontitis — a more serious condition involving irreversible bone loss.

Understanding Gingivitis and Gum Disease
Gingivitis is inflammation of the gums caused by bacterial plaque accumulating at the gumline. It is the earliest and only reversible stage of gum disease. Untreated, it advances to periodontitis, which involves irreversible destruction of the bone and connective tissue supporting the teeth.
The Impact of Plaque Buildup
Plaque is a sticky biofilm that forms continuously on all tooth surfaces. When not removed through daily brushing and flossing, it mineralizes into tartar — a hard calcified deposit that cannot be removed at home. According to the Cleveland Clinic, dentists remove tartar using specialized instruments during professional cleanings. The NIDCR estimates that nearly 47% of adults over 30 have some form of periodontal disease.Age GroupPrevalence of Gum Disease30 and older~47%65 and older~70%
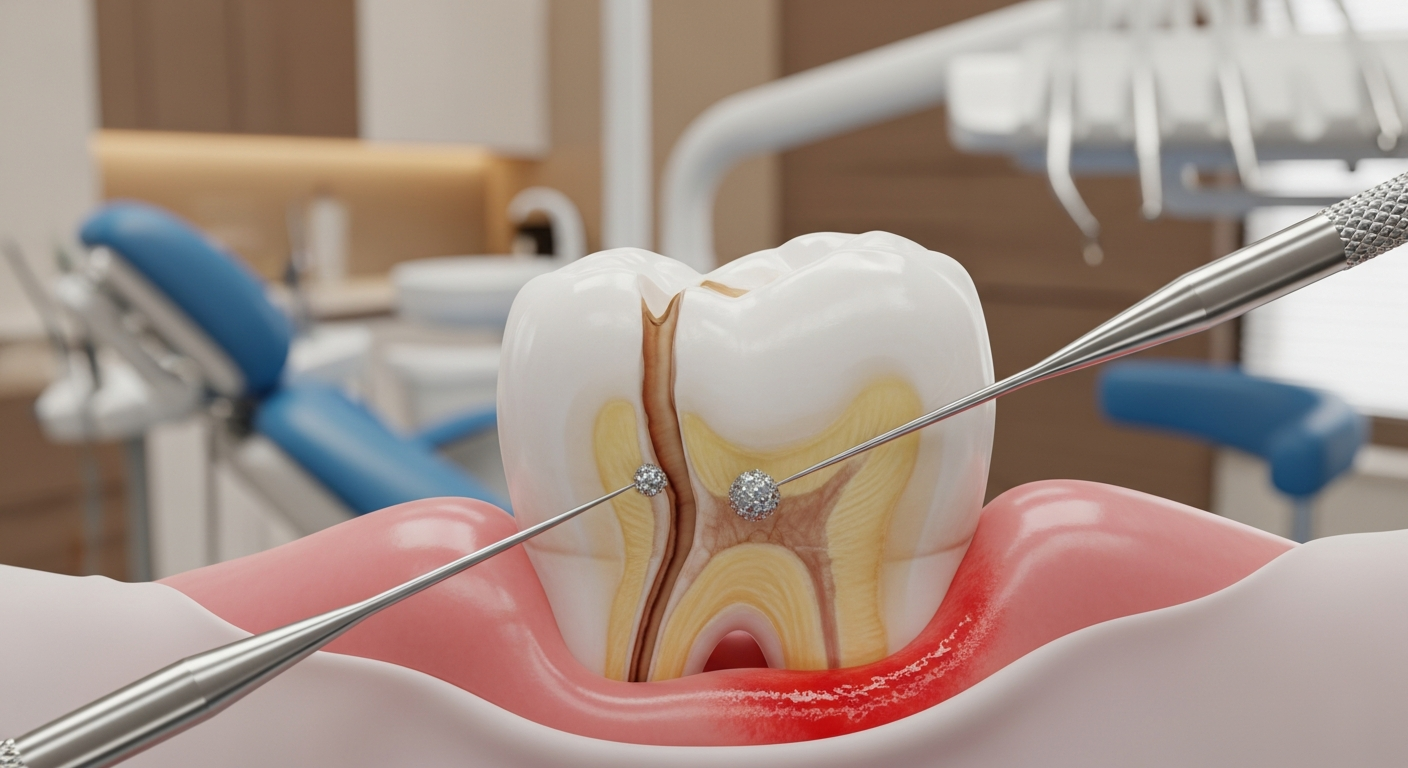
Progression from Gingivitis to Periodontitis
Gingivitis is confined to gum tissue and is reversible. Periodontitis has extended below the gumline to affect the periodontal ligament and alveolar bone — and bone loss is irreversible. Symptoms warranting evaluation include red or swollen gums, bleeding when brushing, persistent bad breath, gum recession, and tooth sensitivity. See also: why you should see a dentist every six months.
Diagnosing Gingivitis
Medical and Dental History Review
Diagnosis begins with a review of the patient’s medical history, particularly conditions affecting immune response or gum health such as diabetes or certain medications. Current oral hygiene habits and any recent changes in gum health are also discussed.
Clinical Examination
The dentist or hygienist uses a periodontal probe to measure pocket depth at multiple points around each tooth. Healthy pockets measure 1 to 3 millimeters. Readings of 4 to 5 millimeters indicate early disease; 6 millimeters or more indicates advanced periodontitis.Pocket Depth (mm)Gum Health Status1–3Healthy4–5Early gum disease6+Advanced periodontitis
Treatment Options for Gingivitis
Non-Surgical Treatment
The foundation of gingivitis treatment is professional cleaning (prophylaxis). The hygienist removes plaque and tartar from all tooth surfaces above the gumline. For patients with pocket depths of 4 to 5 millimeters, scaling and root planing — a more intensive cleaning that extends below the gumline — is performed under local anesthetic.Treatment MethodDescriptionProphylaxisPlaque and tartar removal above gumlineScaling and root planingDeep cleaning below gumline on root surfacesAntibioticsOral or locally delivered to reduce bacterial load
Most patients with gingivitis respond fully to professional cleaning and improved home care. Tissue heals within days to weeks with consistent treatment.
Surgical Interventions for Advanced Cases
When disease has progressed to periodontitis with significant bone loss, surgical intervention may be necessary.ProcedurePurposeFlap surgeryDirect access to deep tartar; bone reshaping if requiredBone graftsReplace lost bone to restore attachment levelSoft tissue graftsRestore receded gum tissue to protect root surfaces
Essential Gum Care
Professional Cleanings
The American Dental Association recommends professional cleanings at least twice yearly for healthy patients. Patients with active periodontal disease typically require three to four visits per year. Tartar can form within 24 to 72 hours on surfaces that are not kept consistently plaque-free — which is difficult to achieve in all areas through home care alone.
Home Oral Hygiene
- Brush: Twice daily, 2 minutes, covering all surfaces
- Floss: Once daily to clean between teeth where plaque accumulates
- Professional cleaning: Every 6 months (or more frequently if recommended)
Diet and Gum Health
Frequent sugar consumption promotes bacterial growth and acid production. Foods that require extensive chewing — firm fruits, vegetables, and raw fibrous foods — stimulate saliva flow which neutralizes acids and delivers minerals to tooth surfaces. Anti-inflammatory dietary patterns including omega-3 fatty acids and limited processed sugar support gum tissue health. For additional detail, see why you should see a dentist every six months.











































.jpg)
.jpg)
























.avif)