Dental Implant Success Rates: What the Evidence Shows

Dental implant success rates consistently exceed 95% at ten years in healthy patients. The primary variables affecting long-term outcomes are jawbone quality, systemic health conditions, smoking status, and the skill of the placing clinician. With proper maintenance, most implants remain functional for 20 years or more.

What “Success Rate” Means Clinically
In implant literature, “survival rate” and “success rate” are distinct measures. Survival rate tracks whether the implant is still in place. Success rate applies stricter criteria: absence of pain, no radiographic bone loss beyond the first year of loading, no infection, and stable soft tissue. Success rates are consistently lower than survival rates, but both measures confirm implants as the most durable tooth replacement option available.
Factors That Affect Success Rate
Jawbone Quality and Density
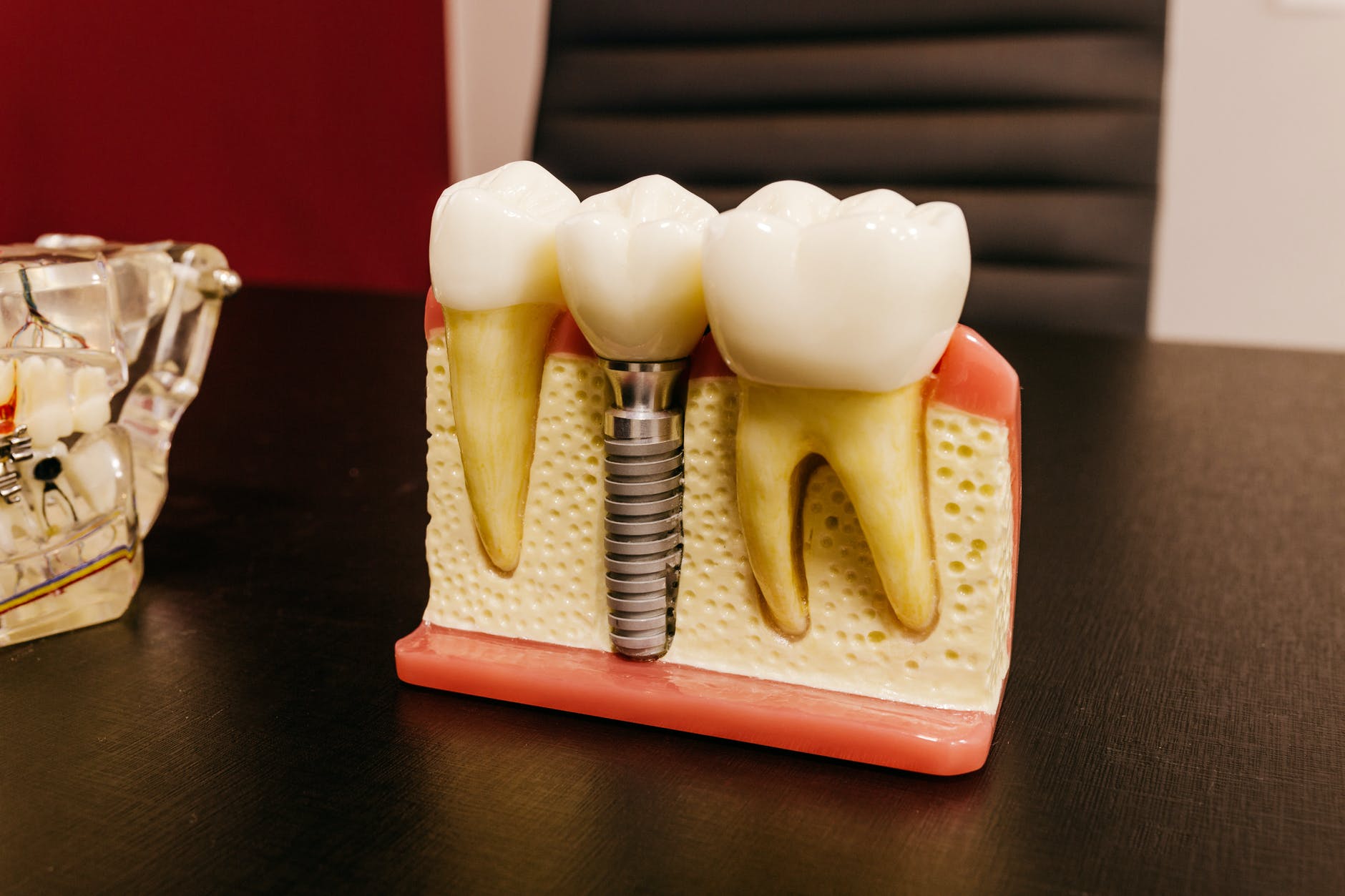
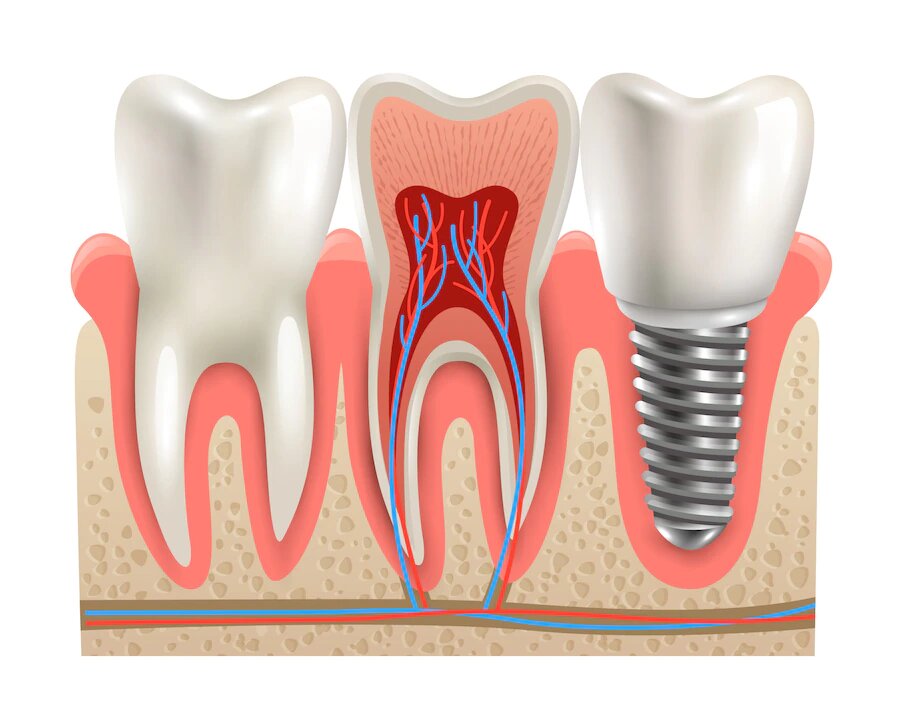
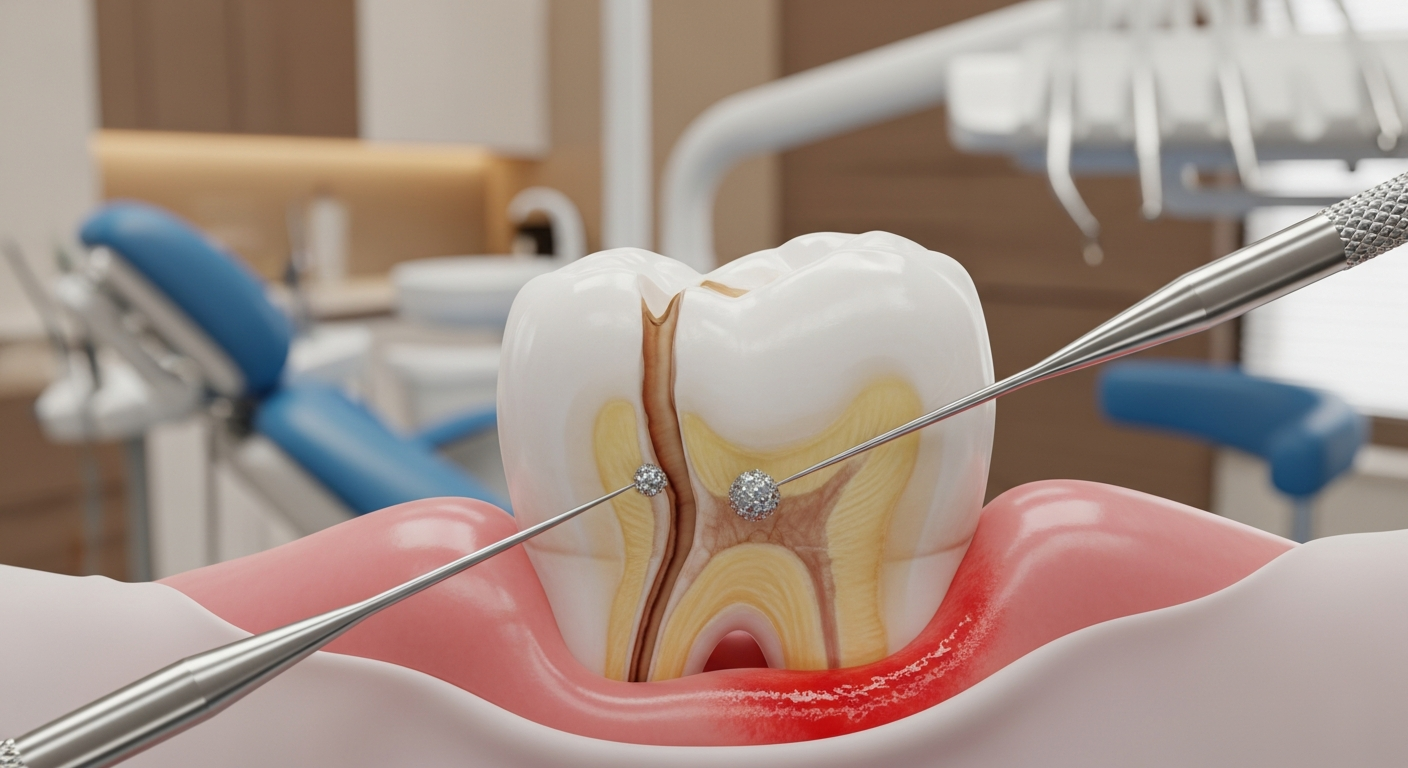
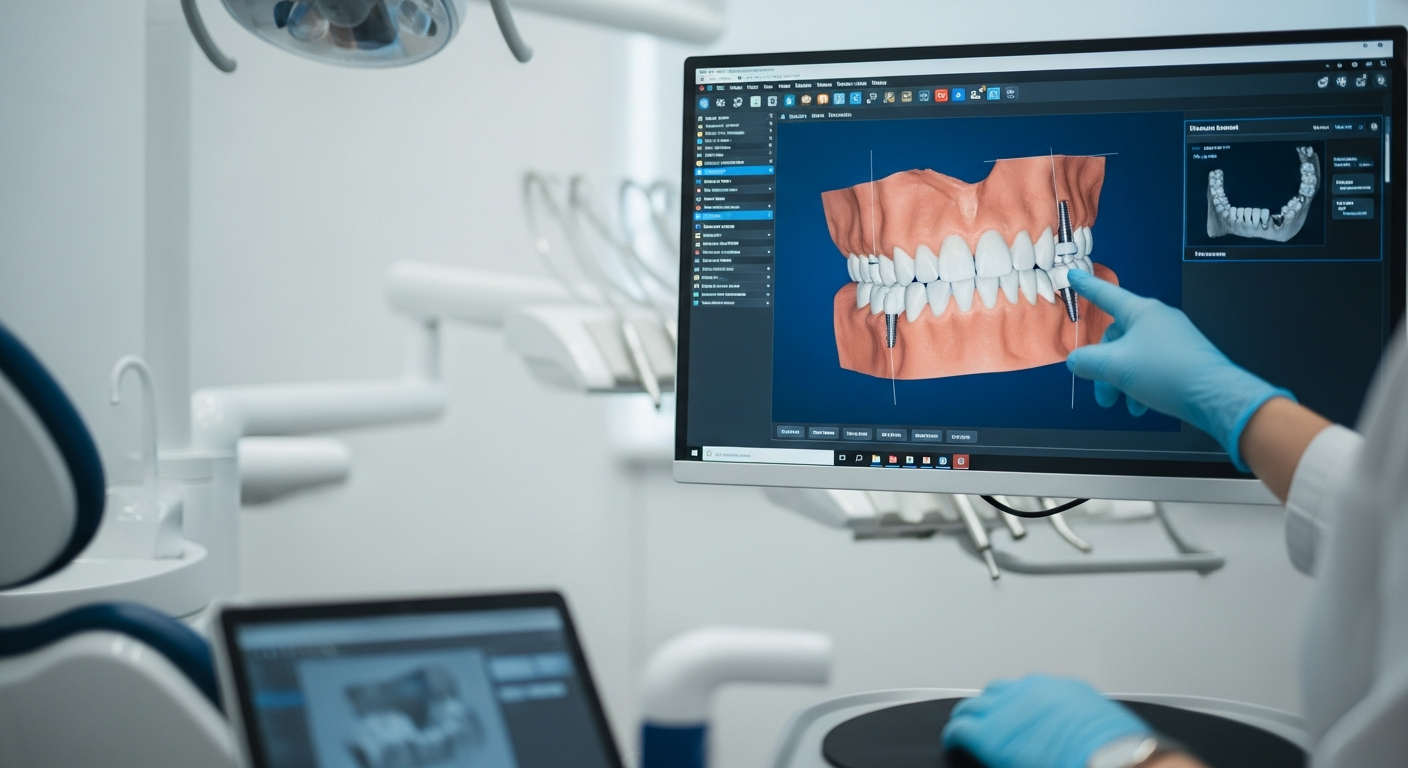
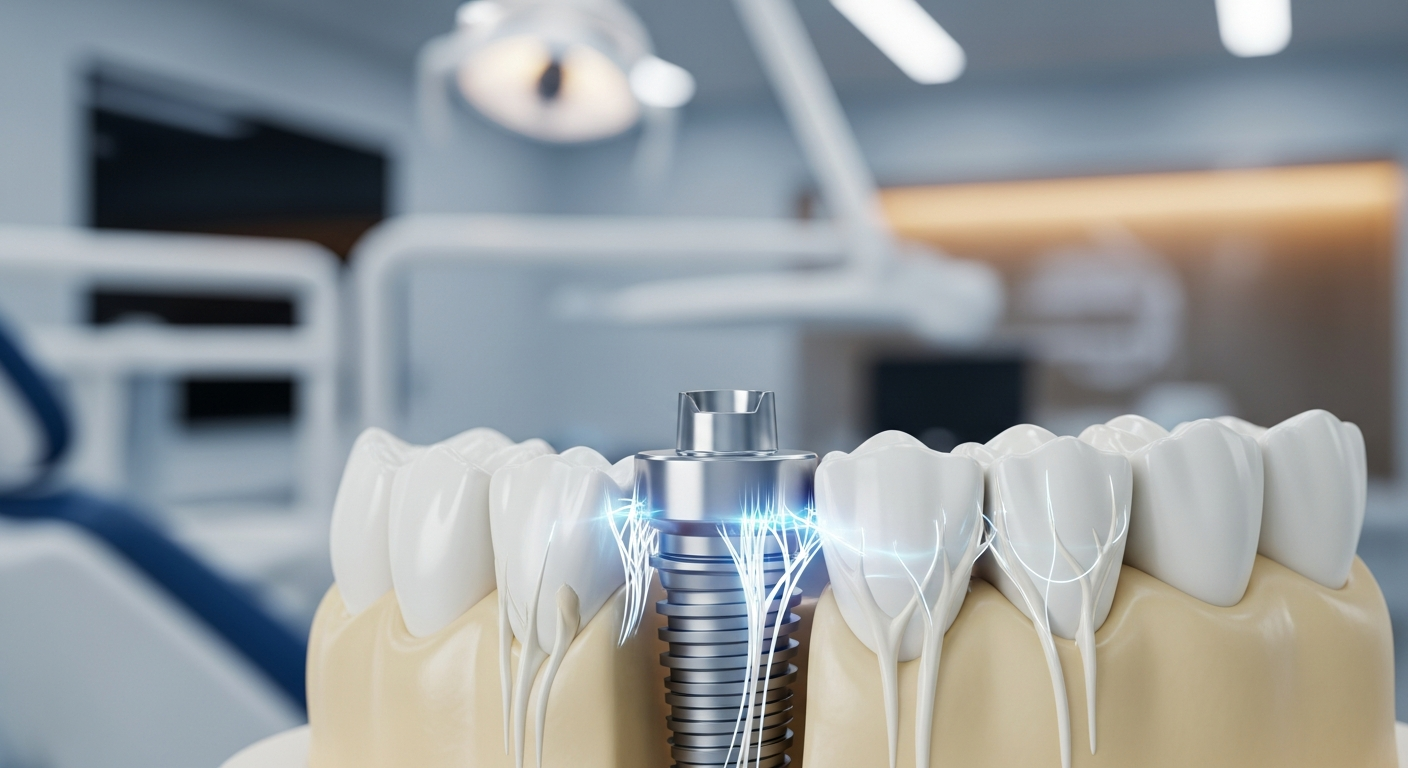
Osseointegration — the fusion of the titanium post with living bone — is the foundation of implant success. Dense cortical bone in the mandible (lower jaw) produces higher success rates than the less dense trabecular bone of the posterior maxilla (upper back jaw). Patients with insufficient bone volume require grafting before placement. CBCT 3D imaging allows precise pre-surgical assessment of bone dimensions.
Bone ConditionImpact on Outcomes
Dense mandibular boneHighest success rates
Posterior maxilla (limited density)Lower success; sinus lift often needed
Adequate volume after graftingSuccess rates comparable to native bone
Insufficient volume without graftingContraindicated
Smoking
Smoking is the most consistently identified behavioral risk factor for implant failure. Nicotine impairs blood flow to healing tissue, slows osseointegration, and significantly increases the risk of peri-implantitis. Patients are counseled to cease smoking at least three months before placement and maintain cessation through the healing period.
Systemic Health
Uncontrolled diabetes impairs healing and increases infection risk. Osteoporosis, particularly in patients taking bisphosphonate medications, requires careful pre-surgical assessment. Most controlled systemic conditions do not disqualify patients from receiving implants but require documentation and coordination with the patient’s physician.
Periodontal History
Patients with a history of periodontitis have higher rates of peri-implantitis — infection around the implant post that causes progressive bone loss. These patients require more frequent maintenance and should be evaluated for bacterial susceptibility before proceeding with implant placement.
Long-Term Maintenance and Monitoring
Implant maintenance parallels natural tooth care. Brush twice daily, floss around the crown margin, and attend professional cleanings every six months. Patients with periodontal history typically require three to four maintenance visits per year. Radiographic assessment of bone levels is performed at clinician-recommended intervals. Early detection of peri-implant bone changes allows intervention before failure occurs.
Maintenance ComponentFrequency
Professional cleaningEvery 6 months (every 3–4 months for perio patients)
Radiographic assessmentAnnually or as directed
Implant mobility checkEvery cleaning visit
Soft tissue evaluationEvery cleaning visit
For more detail on the post-surgical recovery phase, see how to speed up recovery after dental implants. For candidacy assessment, see are you a candidate for dental implants?








































.jpg)
.jpg)
























.avif)